Gluten Sensitivity Skin Symptom Checker
Select the facial or skin changes you have experienced recently that seem linked to eating wheat, barley, or rye.
Select symptoms above
to see your assessment
Assessment Result
--
Recommended Next Step:
- Keep a food diary for 2 weeks
- Consult a gastroenterologist
- Consider an elimination diet
You’ve probably seen the term floating around social media: “gluten face.” It sounds like a specific condition you can diagnose by looking in the mirror. But here’s the truth-there is no medical diagnosis called “gluten face.” Instead, it’s a colloquial term used to describe a cluster of skin and facial changes that often accompany gluten sensitivity or celiac disease.
When people talk about this phenomenon, they aren’t describing a new type of rash. They are usually referring to puffiness, dullness, acne breakouts, or dry patches that seem to appear after eating wheat, barley, or rye. If you’ve noticed your face looking swollen or irritated after a big pasta night, you might be wondering if gluten is the culprit. Let’s break down what actually happens to your body-and your face-when you consume gluten if you have an intolerance.
The Real Meaning Behind "Gluten Face"
First, let’s clear up the confusion. Doctors don’t use the phrase “gluten face” in clinical settings. You won’t find it in any medical textbook. The term emerged from online communities where people shared their experiences with non-celiac gluten sensitivity (NCGS). For these individuals, eating gluten triggers systemic inflammation that manifests visibly on the skin.
So, when someone asks, “What does a gluten face look like?” they are really asking about the visible side effects of gut inflammation. The most common characteristics include:
- Puffiness or Bloating: This isn’t just stomach bloat. Systemic inflammation can cause fluid retention, making your cheeks and under-eye area look puffy.
- Dull, Sallow Skin: Poor nutrient absorption due to gut damage can leave your complexion looking tired and grayish.
- Acne Breakouts: Inflammation can trigger hormonal imbalances and skin irritation, leading to cystic acne, particularly along the jawline and chin.
- Dryness and Eczema: Some people experience flaky, itchy patches as their immune system reacts to gluten proteins.
If you see these symptoms consistently appearing after meals containing wheat, it’s worth investigating further. However, remember that many other factors-like stress, lack of sleep, or dairy consumption-can cause similar issues.
Why Gluten Affects Your Skin
To understand why your face changes, we need to look at what’s happening inside your gut. For people with Celiac Disease, an autoimmune disorder where ingestion of gluten leads to damage in the small intestine, the reaction is severe. When gluten enters the digestive tract, the immune system attacks the lining of the intestines. This damage prevents proper absorption of vitamins and minerals essential for healthy skin, such as zinc, iron, and vitamin D.
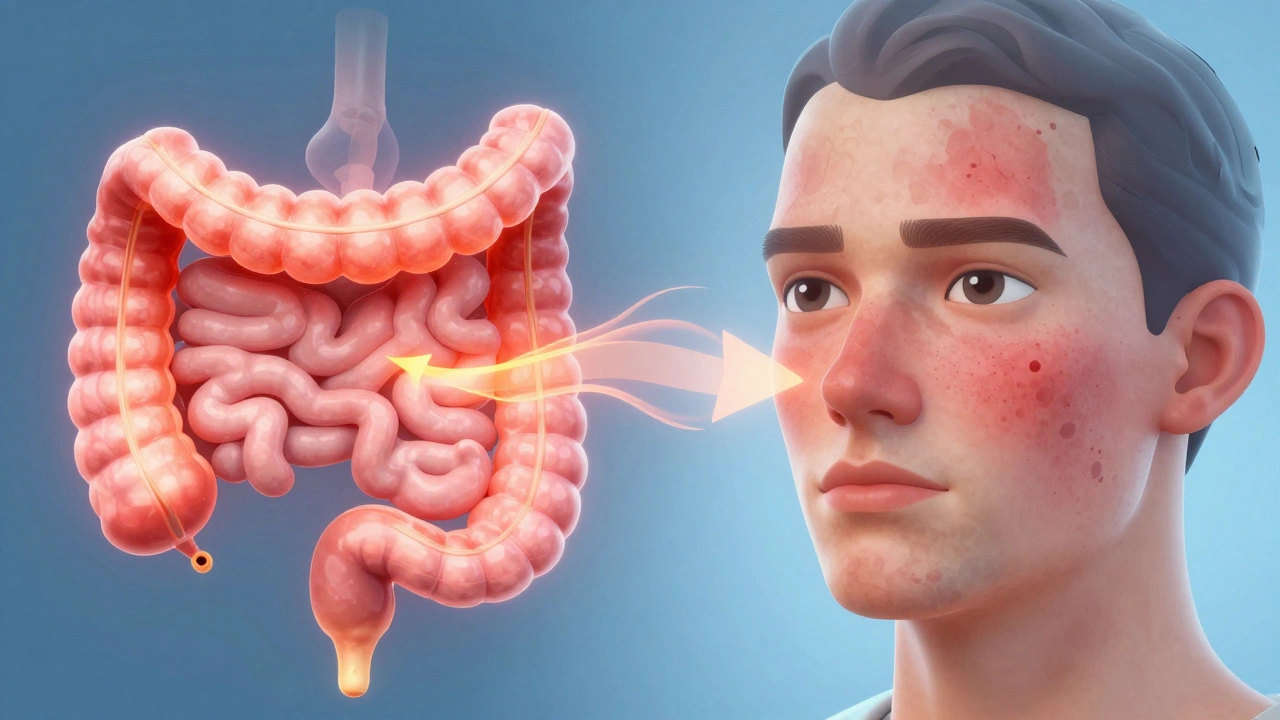
But even if you don’t have Celiac disease, you might have non-celiac gluten sensitivity. In this case, your body still produces an inflammatory response. Think of inflammation as a fire burning inside your body. When that fire spreads, it affects every organ system, including your skin. Your skin is your largest organ, so it’s often the first place where internal distress shows up.
Here’s how the connection works:
- Gut Permeability: Gluten can increase intestinal permeability (often called “leaky gut”), allowing toxins and undigested food particles to enter the bloodstream.
- Immune Response: Your immune system flags these particles as threats, triggering histamine release and inflammation.
- Skin Manifestation: This systemic inflammation can clog pores, disrupt oil production, and cause swelling, resulting in the “gluten face” appearance.
It’s not magic; it’s biology. If your gut is struggling, your skin will likely reflect that struggle.
Common Skin Conditions Linked to Gluten
While “gluten face” is a vague term, several specific dermatological conditions have strong links to gluten consumption. Recognizing these can help you identify if gluten is affecting your appearance.
| Condition | Description | Link to Gluten |
|---|---|---|
| Dermatitis Herpetiformis | An intensely itchy, blistering skin rash. | Considered the cutaneous manifestation of Celiac disease. Occurs in about 10-15% of Celiac patients. |
| Acne Vulgaris | Clogged pores, pimples, and cysts. | Inflammation from gluten can exacerbate hormonal acne, especially in sensitive individuals. |
| Eczema (Atopic Dermatitis) | Dry, red, itchy patches of skin. | Some studies suggest a correlation between gluten sensitivity and eczema flare-ups. |
| Rosacea | Redness and visible blood vessels on the face. | Inflammatory responses to gluten may worsen rosacea symptoms in some cases. |
| Psoriasis | Scaly, silver-colored plaques. | A subset of psoriasis patients report improvement on a gluten-free diet, though evidence is mixed. |
If you suffer from any of these conditions, keeping a food diary can help you spot patterns. Note what you eat and how your skin reacts over the next 24 to 72 hours. Often, the connection isn’t immediate-it takes time for inflammation to build up and show on your face.
Is It Really Gluten? Other Culprits to Consider
Before you throw out all your bread and pasta, consider this: gluten might not be the only thing causing your skin issues. Many people confuse gluten sensitivity with reactions to other components found in wheat products.
FODMAPs: Wheat contains fermentable oligosaccharides, disaccharides, monosaccharides, and polyols (FODMAPs). These carbs can cause bloating and gut distress in people with Irritable Bowel Syndrome (IBS), which might indirectly affect skin health through stress and poor digestion.
Additives: Processed foods often contain preservatives, sugars, and artificial colors that trigger inflammation more than gluten itself. A bagel might make your face puff up, but is it the gluten or the refined flour and yeast?
Dairy: Bread and pizza often come with cheese or milk. Dairy is a far more common trigger for acne and puffiness than gluten. If you’re eating gluten-heavy meals that also include dairy, you might be blaming the wrong ingredient.
To isolate gluten as the cause, you’d need to eliminate it entirely while keeping other variables constant. This is difficult without professional guidance, which is why self-diagnosis can be tricky.
How to Clear Up "Gluten Face" Naturally
If you suspect gluten is behind your skin struggles, here’s a practical approach to finding relief. Remember, I’m not a doctor, so always consult a healthcare provider before making drastic dietary changes.
1. Try an Elimination Diet
The most effective way to know if gluten affects you is to remove it completely for 30 days. During this time, avoid wheat, barley, rye, and hidden sources like soy sauce or malt vinegar. Pay attention to your skin. Do the puffiness go down? Does your complexion brighten? After 30 days, reintroduce gluten and observe if symptoms return. This “challenge” phase confirms the link.
2. Focus on Gut Healing
If you do have a sensitivity, healing your gut is key. Incorporate probiotic-rich foods like yogurt (if you tolerate dairy), kefir, sauerkraut, and kimchi. These help restore healthy gut bacteria, reducing inflammation from the inside out. Bone broth is another excellent option, rich in collagen and amino acids that support intestinal lining repair.
3. Hydrate and Detox
Inflammation thrives in dehydrated bodies. Drink plenty of water to help flush out toxins and reduce puffiness. Adding anti-inflammatory herbs like turmeric, ginger, and green tea to your daily routine can also soothe internal fires that manifest on your skin.
4. Skincare Adjustments
While you heal internally, treat your skin gently. Use non-comedogenic moisturizers and avoid harsh exfoliants that can irritate inflamed skin. Look for products with calming ingredients like aloe vera, chamomile, and niacinamide.

When to See a Doctor
Self-treating with a gluten-free diet isn’t always the right move. If you have Celiac disease, getting tested before going gluten-free is crucial. Once you stop eating gluten, your test results may become inaccurate, delaying a proper diagnosis. Untreated Celiac disease can lead to serious long-term health issues, including osteoporosis, anemia, and neurological problems.
If you experience severe symptoms like chronic diarrhea, unexplained weight loss, or persistent fatigue alongside skin changes, see a gastroenterologist. They can perform blood tests for tissue transglutaminase antibodies and refer you for an endoscopy if needed.
For those with non-celiac gluten sensitivity, there’s no definitive test. Diagnosis is often based on symptom improvement after eliminating gluten. Work with a registered dietitian to ensure you’re getting enough fiber, iron, and B vitamins, which are commonly lacking in gluten-free diets.
Living Gluten-Free Without Sacrificing Flavor
Going gluten-free doesn’t mean giving up taste. In fact, many people discover that fresh, whole foods taste better than processed alternatives. Swap white bread for almond flour or oat-based options. Replace pasta with zucchini noodles or chickpea pasta. There are countless delicious recipes that naturally exclude gluten while nourishing your body.
Experiment with spices, herbs, and healthy fats to add depth to your meals. Avocado, olive oil, and nuts provide satiety and nutrients that support skin health. By focusing on quality ingredients, you’ll likely notice your “gluten face” clearing up within weeks.
Your skin is a reflection of your internal health. If you’ve been battling puffiness, acne, or dullness, it might be time to listen to your body. Whether it’s gluten or something else, identifying the root cause is the first step toward glowing, healthy skin.
Does everyone get a "gluten face"?
No. Only people with gluten sensitivity, Celiac disease, or non-celiac gluten sensitivity may experience skin changes linked to gluten consumption. Most people digest gluten without any adverse effects on their skin or overall health.
How long does it take for "gluten face" to go away?
For many people, skin improvements start within 2 to 4 weeks of eliminating gluten. However, complete gut healing can take months, especially in cases of Celiac disease. Consistency is key to seeing lasting results.
Can drinking beer cause "gluten face"?
Yes, if the beer contains gluten (like traditional lagers and ales) and you have a sensitivity. Alcohol also dehydrates the body and causes inflammation, which can worsen puffiness and skin clarity regardless of gluten content.
Is "gluten face" permanent?
No. The symptoms associated with gluten sensitivity are reversible. Once you remove the trigger and allow your gut to heal, your skin should return to its normal state. Long-term damage only occurs if the underlying condition remains untreated for years.
Should I go gluten-free if I don't have Celiac disease?
Not necessarily. Unless you have diagnosed sensitivity or Celiac disease, gluten is generally safe. Going gluten-free unnecessarily can lead to nutritional deficiencies and higher costs. Focus on a balanced diet rich in whole foods instead.

